Drs. Gregori M. Kurtzman and Douglas F. Dompkowski illustrate an approach that can avoid complications
Introduction
The posterior maxilla presents with a common problem clinically following tooth extraction or crestal bone loss resulting in loss of osseous height sufficient to place implants.
[userloggedin]
Resorptive patterns in some patients along with sinus enlargement result in minimal bone that can accommodate implant placement. Maxillary sinus augmentation over the past 18 years with various bone graft materials has become routine treatment.
Numerous studies have reported highly successful implant survival rates when placed into the augmented sinus.¹-3 Transalveolar sinus floor elevation, also referred to as subantrial augmentation, was first described by Tatum4 and later modified by Summers.5-7 This technique utilized a series of osteotomes with a mallet to create an osteotomy and subsequent in-fracturing of the sinus floor while elevating the Schneiderian membrane. Following manipulation, the space created in the sinus is augmented with various bone particulate graft materials, increasing the volume of bone available for implant placement. 
Various studies have reported that when 5 mm of residual alveolar bone is present, simultaneous implant placement can be performed to achieve adequate primary stability.6,8,9 But when less than 5 mm of residual alveolar bone height is available, a delayed two-stage approach has been recommended.10,11 The most common complication of the lateral sinus elevation approach is typically tearing of the Schneiderian membrane, which could allow for bacterial contamination or loose particles to gain access to the sinus cavity.
A safer lateral window approach sinus augmentation procedure will be discussed using specialized safe cutting end drills with vertical stoppers for osseous window formation and subsequent membrane elevation (Lateral Approach-Sinus Kit (LASK), HIOSSEN).
Materials and methods
The LASK provides dome drills, core drills, metal stoppers, a side wall drill, and a bone separator tool (Figure 1).
The dome drill is a unique osseous drill allowing removal of the lateral wall of the maxillary sinus while collecting autogenous bone to be added to the material to be placed into the sinus. Macro- and micro-cutting blades provide excellent cutting of the lateral wall without tearing of the sinus membrane. These dome drills, available in both 5.0 and 7.0 mm in diameter, are run at 1,200 to 1,500 rpm with irrigation in an implant surgical handpiece. Metal depth control stoppers are provided that fit on the dome drills, limiting depth of penetration (0.5, 1.0, 1.5, 2.0, 2.5, and 3.0 mm) and are used sequentially to safely expose the sinus membrane.
The core drill, also available in 5.0 and 7.0 mm diameter differs from the dome drill in that the center does not cut, with bone removal resulting in a core of bone being left over the sinus. This bony lid may be elevated with the sinus membrane still attached becoming the new “roof” to the sinus with osseous augmentation being placed below it. This particular drill follows the same design of the CAS-Kit (crestal augmentation sinus) drills and are utilized at 1,200-1,500 rpm. The metal drill stoppers also fit these drills, allowing controlled sequential depth preparation. The bone separator tool is utilized to separate the osseous core created with the core drill if removal is desired and is based on the practitioner’s preferred technique.
The side wall drill may be used to enlarge the osseous window created by the dome drill if desired. The tip of this drill is smooth and designed to safely push the sinus membrane away from the cutting portion of the drill, which starts 1 mm from the safe end. Osseous cutting is performed at 1,500 rpm, using the side of the rotating drill to enlarge the osseous window. The CAS-Kit metal drill stoppers may be placed on this drill to limit accidental penetration too far into the sinus and tearing of the membrane during this drill’s use. As with the other drills in this kit, irrigation is needed during its use.
Case report
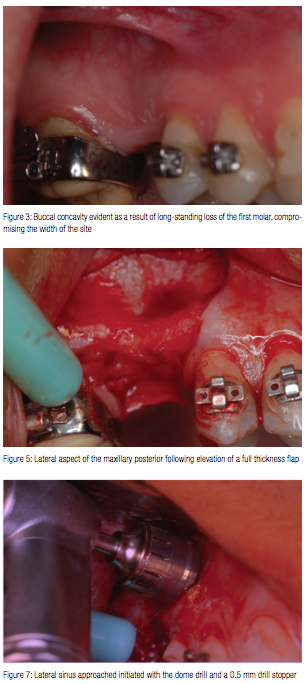
A 32-year-old male presented with the desire for implant placement in the posterior maxillary right quadrant which had been missing the first molar for an extended period of time. The result of long-term loss of the tooth resulted in drifting of the second molar into the space, which was corrected orthodontically prior to implant surgery. Radiographically, enlargement of the maxillary sinus was noted with insufficient height in the molar region for implant placement (Figure 2). Resorption was noted compromising the width of the ridge at the buccal leading to a mild concavity (Figure 3). Sinus augmentation was discussed to assist in achieving the patient’s desired treatment goal of implant placement and restoration with a fixed crown.
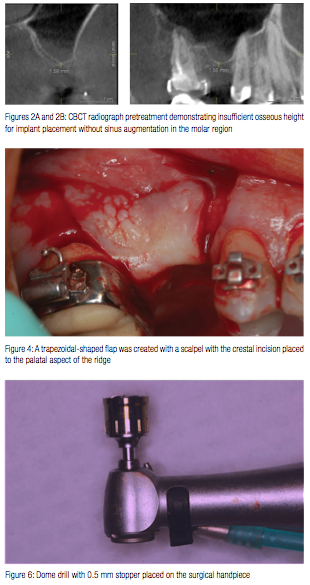
Following administration of local anesthetic, a crestal lingual incision was made with vertical releasing incisions at the mesial and distal aspect of the site, and a full thickness flap was elevated, leaving the attached gingiva undisturbed on the adjacent teeth (Figure 4). Elevation of the flap extended superiorly to expose the lateral wall of the maxillary sinus up to the inferior aspect of the zygoma (Figure 5).
A 0.5 mm wide dome drill was placed onto the surgical handpiece with a 0.5 mm drill stopper (Figure 6). This would allow initiation of the window without the possibility of excessive penetration and subsequent damage to the sinus membrane. The initial dome drill is placed onto the surgical handpiece with the selected drill stop. The dome drill with stopper was placed on the lateral sinus wall at a height more superior then the current height of the available bone as measured radiographically (Figure 7). This is done to ensure that the window created has elevated the membrane circumferentially.
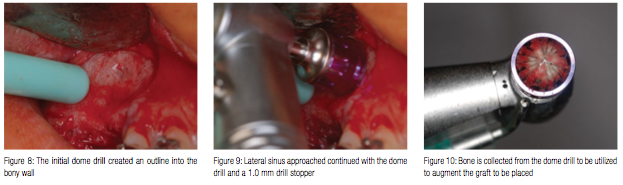
When maximum depth has been achieved with the 0.5 mm drill stopper present, the drill stopper is changed to a 1.0 mm stopper, and drilling is continued (Figure 8). The drill stopper is sequentially increased while checking for membrane exposure. Lateral drilling continues stepping up to the next drill stop (Figure 9). Bone collected on the dome drills is removed from the drill and placed into a sterile dish to be added to the graft to be placed, adding the host’s osteopotential cells to the graft (Figure 10). As bone is removed over the sinus membrane, the area changes in color from the light color of the bone (ivory) to darker gray as the dark sinus begins to show clinically at the window (Figure 11).
Final window creation is made with the dome drill, in this particular case with a 2.5-mm drill stopper (Figure 13). Some patients may require deeper drilling, which is dependent on thickness of the lateral maxillary sinus wall. The intact sinus membrane is noted with no bone over the membrane at the window that has been created on the lateral wall (Figure 14). Additionally, host bone is collected from the dome drill.
Sinus curettes are utilized to start the sinus membrane elevation at the inferior aspect, teasing the membrane from the osseous wall of the sinus interiorly (Figure 15). Following elevation of the membrane, the membrane should be intact and free of visible tears that may prevent graft distribution within the sinus during initial healing (Figure 16). It is important that the elevation also include the medial wall of the sinus so that it fills a volume great enough that the implant, when placed, will be surrounded by bone. Failure to elevate the medial aspect may result in the implant, when placed, having no osseous contact, which may decrease clinical success following loading. Additionally, the authors advise elevation to a greater height then the implant length to be placed when a delayed fixture placement is to be performed. This will allow for possible graft settling during healing that may yield less height than was planned.
An absorbable extracellular membrane (DynaMatrix®, Keystone Dental) is inserted into the sinus to act asprotection, containing the graft material and thickening the sinus membrane, and sealing any micro tears that might be present (Figure 17). The resorbable membrane is cut to size and placed into the sinus dry using the patient’s blood in the site to wet it as it is placed. Once wetted with blood, the resorable membrane becomes sticky, gluing itself to the sinus membrane.

Regenaform® cortical cancellous bone chips (Exactech®) and SureOss®, a freeze-dried cortical allograft (HIOSSEN) were used in a 50:50 ratio in a sterile dappen dish and mixed with the autogenous bone collected from the dome drill. The osseous graft mixture was carried to the oral cavity, introduced into the elevated sinus, and gently condensed with a large plugger, pushing the mixture to the medial wall and filling in a lateral direction until the entire cavity was filled (Figure 18). The process was repeated in the cavity anterior to the septa. Sufficient osseous graft was placed till the sinus was augmented to be flushed with the outer aspect of the lateral sinus wall at the window that had been created (Figure 19).

Following sinus grafting, the site was prepared, and an implant (4.5 x 10 mm, ETIII, HIOSSEN) was placed at the site. A low profile cover screw was used to allow primary closure of the flap. The radiograph shows initial graft placement and the elevation achieving a site that can accommodate implant placement at this surgical appointment (Figure 20).
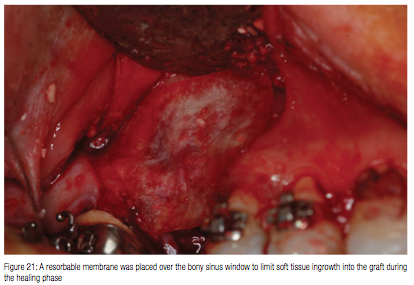
A long-term resorbable membrane (DynaMatrix) was cut to extend beyond the outline of the lateral window and placed over the osseous graft that had been placed into the sinus (Figure 21). The flap was repositioned and initially closed with a horizontal mattress suture using a 5-0 Cytoplast™ suture material, (Osteogenics Biomedical) to achieve primary closure of the flap without tension, and then the crest was closed with interrupted sutures (Figure 22). This suture serves to resist soft tissue tension that may result due to inflammation and the resulting swelling following surgery. Additional sutures are placed to close the incision line using a simple interrupted technique.

The patient returned 8 months after implant placement. Soft tissue in the site on the lateral aspect demonstrated no inflammation, and incision lines were not discernible on the gingiva. The implant was exposed using a disposable tissue punch, and the cover screw was replaced by a healing abutment. A radiograph was taken to check and verify the organization of the osseous graft that had been placed into the sinus, integration of the implant, and seating of the healing abutment on the fixture (Figure 23). A CBCT was taken to check the graft and implant integration, and the implant was ready to be restored (Figure 24).
Conclusion
Emphasis has moved to the use of a crestal approach to sinus elevation when additional osseous height is required for implant placement. This approach works well when at least 5 mm of osseous height is present for immediate implant placement. Yet, when less bone height is present, a lateral window approach may be the preferred technique to increase crestal height and geometric volume so that implant fixtures may be placed.
The lateral sinus augmentation approach can be challenging as tearing of the sinus membrane often necessitates abandoning the procedure and re-entry at a later date after the membrane has healed. Previous techniques involved use of diamonds or carbides in a high-speed handpiece or the use of peizo surgical units. These approaches had potential for membrane damage (burs in a high speed) or were very slow (peizo). The LASK from HIOSSEN utilizes specially designed drills that greatly minimize tearing of the membrane and improve the safety of the procedure.
REFERENCES
1. Blomqvist JE, Alberius P, Isaksson S. Two-stage maxillary sinus reconstruction with endosseous implants: A prospective study. Int J Oral Maxillofac implants. 1998;13(6):758-766.
2. Valentini P, Abensur DJ. Maxillary sinus grafting with anorganic bovine bone: A clinical report of long-term results. Int J Oral Maxillofac Implants. 2003;18(4):556-560.
3. Tong DC, Roux K, Drangsholt M, Beirne OR. A review of survival rates for implants placed in grafted maxillary sinuses using META analysis. Int J Oral Maxillofac Implants. 1998;13(2):175-182.
4. Tatum OH Jr. Maxillary and sinus implant reconstructions. Dent Clin North Am. 1986;30(2):207-229.
5. Rosen PS, Summers R, Mellado JR, Salkin LM, Shanaman RH, Marks MH, Fugazzotto PA. The bone-added osteotome sinus floor elevation technique: multicenter retrospective report of consecutively treated patients. Int J Oral Maxillofac Implants. 1999;14(6):853-858.
6. Summers RB. A new concept in maxillary implant surgery: the osteotome technique. Compendium. 1994;15(2):152-162.
7. Summers RB. The osteotome technique: Part 3—Less invasive methods of elevating the sinus floor. Compendium. 1994;15(6):698-710.
8. Emmerich D, Att W, Stappert C. Sinus floor elevation using osteotomes: a systemic review and meta-analysis. J Periodontol. 2005;76(8):1237-1251.
9. Toffler M. Osteotome- mediated sinus floor elevation: a clinical report. Int J Oral Maxillofac Implants. 2004;19(2): 266-273.
10. Peleg M, Mazor Z, Chaushu G, Garg AK. Sinus floor augmentation with simultaneous implant placement in the severely atrophic maxilla. J Periodontol. 1998;69(12):1397-1403.
11. Peleg M, Mazor Z, Garg AK. Augmentation grafting of the maxillary sinus and simultaneous implant placement in patients with 3 to 5 mm of residual alveolar bone height. Int J Oral Maxillofac Implants. 1999;14(4):549-556.
Stay Relevant With Implant Practice US
Join our email list for CE courses and webinars, articles and mores

 Drs. Gregori M. Kurtzman and Douglas F. Dompkowski illustrate an approach that can avoid complications
Drs. Gregori M. Kurtzman and Douglas F. Dompkowski illustrate an approach that can avoid complications
