Dr. Cary Shapoff discusses the great clinical significance of narrow implants for practitioners in private practice
In my practice, I encounter patients with congenitally missing maxillary lateral incisors and fractured maxillary and mandibular incisors.
[userloggedin]
These sites often present restricted dimensions not only buccolingually but also interproximally. In the past, loss of a single lower incisor often created the need for extensive fixed restorative care.
Congenitally missing lateral incisors, often restored with bonded bridges, have the untoward consequence of frequent debonding. Narrow implants may serve as a provisional anchoring device to protect the site during a traditional implant healing phase. The use of the narrow dental implant now allows the clinician to treat most of these specific sites with the conservative alternative of the single dental implant compared to the need for extensive fixed restorative care. Occasionally, other forms of interdisciplinary care need to be considered prior to or in conjunction with the placement of dental implants.
Since the advent of dental implants as an alternative for replacing missing teeth or replacing damaged existing teeth, the development of numerous implant styles and sizes has improved our ability to treat sites otherwise considered compromised. Narrow dental implants are available as a one-piece fixture or traditional two-piece. The advantages of the two-piece implant include the opportunity to allow delayed loading and the flexibility of using different prosthetic components. My choice has been the BioHorizons® Tapered Internal 3.0 implant as well as the small diameter 3.5 mm platform implant for restricted spaces. These implants offer prosthetic abutment choices with a variety of provisional abutments, stock abutments, and CAD/CAM titanium or ceramic abutments with Laser-Lok® microchannels. This microchannel technology on the collar allows for enhanced soft tissue “functional” attachment to the abutment surface.
This article describes the use of narrow implants in a variety of common clinical situations and a discussion of the treatment sequence and modalities utilized for each case. Each of the cases presented in this article provided different surgical and restorative challenges.
Case 1
 A 44-year-old female was seen for dental implant consultation for tooth No. 26 in December 2009. She has previously had tooth No. 26 extracted 6 months earlier without socket grafting (Figure 1). The existing alveolar ridge was narrow and required additional bone augmentation to improve the ridge dimension (Figure 2). Five months after ridge grafting, a BioHorizons 3.0 mm implant (3.0 x 12 mm) was placed and allowed to heal for 3 additional months (Figures 3, 4, and 5). Following second-stage surgery, a screw-retained provisional crown was placed to shape the gingival tissue (Figure 6). The final crown was placed 10 weeks later. Figures 7 and 8 represent the 3-year follow-up visit (July 2013) with a custom cast UCLA abutment and EMAX crown. Metallic abutment show-through was evident on the thin marginal tissue. The 3.0 Ti-Base CAD/CAM milled ceramic abutment became available after restoration of this implant. This case represented the first clinical anterior restoration of the BioHorizons 3.0 implant in private practice (restoration by Dr. David Wohl, Fairfield, Connecticut).
A 44-year-old female was seen for dental implant consultation for tooth No. 26 in December 2009. She has previously had tooth No. 26 extracted 6 months earlier without socket grafting (Figure 1). The existing alveolar ridge was narrow and required additional bone augmentation to improve the ridge dimension (Figure 2). Five months after ridge grafting, a BioHorizons 3.0 mm implant (3.0 x 12 mm) was placed and allowed to heal for 3 additional months (Figures 3, 4, and 5). Following second-stage surgery, a screw-retained provisional crown was placed to shape the gingival tissue (Figure 6). The final crown was placed 10 weeks later. Figures 7 and 8 represent the 3-year follow-up visit (July 2013) with a custom cast UCLA abutment and EMAX crown. Metallic abutment show-through was evident on the thin marginal tissue. The 3.0 Ti-Base CAD/CAM milled ceramic abutment became available after restoration of this implant. This case represented the first clinical anterior restoration of the BioHorizons 3.0 implant in private practice (restoration by Dr. David Wohl, Fairfield, Connecticut).
Case 2
A 67-year-old male was referred for generalized periodontal care prior to a maxillary full-arch rehabilitation with a new bridge to replace a failed restoration. In addition to generalized, moderate to severe periodontitis, the patient demonstrated a periodontal abscess with severe bone loss on tooth No. 24, and was given a hopeless prognosis (Figures 9-10). He also demonstrated clinical signs of bruxism with significant incisal and occlusal wear. Numerous restorative options were discussed with the patient for site No. 24. A single dental implant with adjacent, full-crown coverage was selected, assuming that the first phase bone grafting procedure would allow proper dimension for implant placement. The patient preferred individual teeth rather than fixed bridgework. A provisional bridge was placed, leaving the root of tooth No. 24 in place (root banking), to prevent soft tissue shrinkage and bone loss secondary to extraction prior to the ridge augmentation procedure.
The surgical procedure consisted of surgical flap entry, debridement of subgingival calculus from all involved teeth, meticulous defect debridement, and ridge augmentation. A combination graft of MinerOss® particulate (mineralized cortical and cancellous bone) and rh-PDGF-BB biologic modifier (Gem-21S®, Osteohealth) was utilized and then covered with a contoured titanium reinforced PTFE barrier (Cytoplast™, Osteogenics Biomedical) and allowed to heal for 6 months (Figure 11). A BioHorizons 3.0 implant was placed (Figure 12) and allowed to heal for an additional 3-month period. After provisionalization of the implant, a final crown was placed on a custom cast abutment (Figures 13-14) (Dr. Jeffrey Babushkin, Trumbull, Connecticut).
Case 3
A 57-year-old female patient presented with localized bone loss and pocketing in the lower anterior region (Figure 15). Tooth No. 25 had previously been surgically treated in another office and veneer restorations were placed on the two central incisors. Tooth No. 24 was rotated with a closed interproximal embrasure. Tooth No. 24 exhibited minimal mobility, but tooth No. 25 was significantly mobile. Various treatment options were discussed with the patient, including fixed bridgework, bonded bridge, replacement of missing teeth with implant-retained restorations. The patient preferred individual tooth replacement with a dental implant but refused extraction and replacement of tooth No. 24. She was presented with a two-phased approach, involving alveolar ridge reconstruction of site No. 25 and re-evaluation of the periodontal status of tooth No. 24. A CBCT was required before treatment plan discussions. The patient also requested a fixed provisional restoration during the treatment phases.
The axial view of the CBCT (Figure 16) clearly demonstrated the significant loss of ridge dimension from the failure of the prior regenerative procedure. Ridge grafting was accomplished with MinerOss cortical and cancellous bone hydrated with rhPDGF-BB. A tenting screw was fixed to the lingual wall of the defect to serve as a support for the graft material and barrier (Figure 17). Bovine pericardium (CopiOs) was used as the barrier material and primary closure of the defect was obtained and maintained with 6-0 propylene sutures. Healing was uneventful, and the patient was seen on a regular post-operative schedule. Following 6 months of successful graft healing, the tenting screw was removed, and a BioHorizons Tapered Internal 3.0 implant (12 mm length) was placed after determining adequate ridge dimension by direct measurement (Figures 18-19). The implant was allowed to heal for an additional 3 months until second-stage surgery and screw-retained provisionalization utilizing a PEEK abutment and composite crown. The tooth was then restored utilizing a 3.0 titanium custom cast abutment and a lithium disilicate crown (Figures 20-21) (restoration by Dr. David Wohl, Fairfield, Connecticut).
Slight metal show-through of the abutment was evident because the patient demonstrated thin biotype, and a connective tissue was performed upon her request.
Case 4
This 47-year-old female recently had a missing maxillary lateral incisor replaced with a long narrow one-piece implant of unknown origin (Figure 22). Unfortunately, the prosthetic platform of the implant was improperly positioned, resulting in the platform being very coronal to the osseous crest and the resulting crown (provisional) being very short and unesthetic (Figure 23). It was determined that despite the recent procedure in another office, the appropriate solution was to remove the existing dental implant, repair the site, and consider another narrow implant, placed at the proper prosthetic level. CBCT radiographic analysis was necessary to determine ridge width and intraosseous implant positioning. After raising a full thickness mucoperiosteal flap on the facial surface, the implant was removed utilizing a vertical cut in the facial wall alveolus with a piezotome handpiece and reverse rotation of the implant with a surgical extraction forcep (Figure 24). The initial plan was to reconstruct the site, allow 4 months of healing, and then place a narrow two-piece dental implant. At the time of the first surgery, the ridge dimension width, the facial location of the initial implant in the alveolus, and the minimal ridge destruction during its removal allowed placement of a BioHorizons 3.0 narrow implant in an ideal position using a surgical guide provided by the prosthodontist. The implant was placed in a more palatal position in the alveolar ridge allowing 2 mm of distance from the implant surface to the facial plane of the alveolus (Figure 25). Allograft bone (MinerOss) was placed in the surgical defect and an additional onlay bone graft was placed and covered with a resorbable collagen barrier. The site was allowed to heal for 4 months before a second-stage surgery and placement of a screw-retained provisional crown to shape the gingival tissue. The final crown and custom abutment were delivered 3 months later (Figures 26-27). (restoration by Dr. Jeffrey O’Connell, Bridgeport, Connecticut)
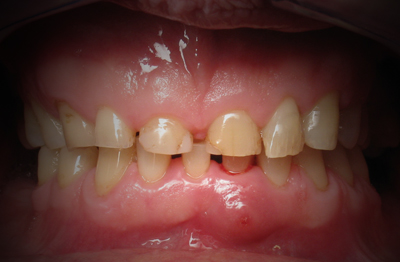
Opportunities to use narrow dental implants can assist the clinician in providing support for interim prosthesis during a bone graft or dental implant healing phase. The case below (Figures 28-31) shows use of a narrow implant (MDL, Ultimatics, Inc.) to support a removable prosthesis and to reduce or eliminate pressure on the surgical site where two BioHorizons Tapered Internal implants (3.5 mm platform) were placed simultaneous to extraction of teeth No. 8 and No. 10 following horizontal fracture of the abutment teeth at the gingival level. The patient had a strong bruxing habit and frequent travel schedule, which negated the consideration of immediate provisionalization. The “provisional implant” was connected to the removable provisional with an “O-ring” in the provisional to provide an axial stop and prevent pressure on the implant and bone graft healing site. (final restoration — Dr. Michael Reynolds, Southport, Connecticut)
Discussion
In all cases presented, various treatment options were discussed with the patients. For example, in Case No. 1, the other restorative options considered for her were bonded bridge or fixed bridgework. Key elements to the success of the restoration appeared to be use of CBCT to allow a three-dimensional view of the bone anatomy, additional grafting to create an adequate ridge, and a screw-retained provisional to support the facial and interproximal gingival contours.
Since the restoration of this case, BioHorizons has introduced the Ti-Base CAD/CAM milled custom ceramic abutment with Laser-Lok microchannels on the abutment margin. These non-random nano-dimensioned (8 micron) grooves have been in clinical practice for 14 years, and enhanced crestal bone maintenance has been demonstrated in the literature by this author, as well as others. In addition, recent human and animal histology (Nevins, et al.) has confirmed an enhanced response of bone and soft tissue to the Laser-Lok surface, providing a “functionally-oriented” attachment of connective tissue to the implant collar, as well as the abutment surface above the implant/abutment connection.
Success of several of these cases was a result of adequate reconstruction of the alveolar ridge and the use of the narrow BioHorizons Tapered Internal Implants (Case No. 2 — 3.5 mm platform, Case No. 3 — 3.0 mm platform). Regeneration of lost alveolar bone involved the use of allograft bone material, biologic modifiers, and space maintaining barriers. In addition, adequate time was necessary to allow graft incorporation and maturation. Selection of the appropriate implant size was also a component of success. Literature suggests that implant site preparation should provide for at least 2 mm of facial bone and at least 1.5 mm of interproximal bone around the implant body. There is an advantage in using an implant system, such as BioHorizons. The system offers various narrow platform dimensions to allow the clinician flexibility in selecting the appropriate implant body size to maintain proper alveolar bone around the implant. Placing the implant too close to the facial bone wall can result in untoward bone resorption, exposure of implant threads, esthetic compromises in thin tissue biotypes, and possibly loss of implant integration. Use of an implant style that has a thread design capable of providing excellent initial biomechanical stability also allows for immediate provisional loading, where appropriate. Proper treatment planning and the use of 3-dimensional imaging are also essential in cases of restricted space. The opportunity to allow sites to heal undisturbed, following bone grafting as in Case No. 4, is a clear advantage of the two-piece narrow dental implant over the one-piece implant. In addition, the variety of prosthetic abutment choices allows for creation of a more ideal contour of the subgingival abutment anatomy resulting in better esthetics and marginal tissue and bone health.
Finally, at the time of this writing, two interesting cases were treated by me on two consecutive days, clearly demonstrating the need and the advantage of using narrow dental implants as part of the implant family of sizes available to the clinician. Both cases, one with crown and root fracture (Figures 32-33) and the other with external root resorption (Figures 34-35) presented with restricted spaces and narrow alveolar anatomy. Both were able to be surgical treated with extraction and simultaneous implant placement.
Today, clinicians tackle complex dental problems with more sophisticated diagnostic procedures and surgical techniques that utilize superior grafting materials and biologic modifiers. Our restorative colleagues utilize intraoral scanning devices to replace impressions and CAD/CAM milling services to create custom-contoured abutments and crowns. The use of narrow dental implants that provide predictable strength and restorative flexibility are an additional “tool in the armamentarium” that offers the clinician the opportunity to treat restricted space situations.
Gallery
{gallery}140310_cl_shapoff{/gallery}
Stay Relevant With Implant Practice US
Join our email list for CE courses and webinars, articles and mores


