Drs. Arun K. Garg and Gustavo Mugnolo illustrate how Garg sticky bone can be used in place of liquid PRP in sinus grafting.
Drs. Arun K. Garg and Gustavo Mugnolo discuss a new formulation to predictably regenerate bone
It has been more than 20 years since Drs. Arun Garg and Robert Marx developed the original formula for platelet-rich plasma (PRP), a vital wound-healing and regenerative agent that today is used by doctors in virtually every field of dentistry and medicine. In dentistry, the biologic assistance provided by PRP can facilitate bone healing under a range of implant-related procedures involving autogenous bone, allogeneic bone, synthetic bone, and bone graft composites. This article describes a technique for using PRP in a unique formulation developed more recently by the authors to predictably regenerate bone and support implant placement without the need for autogenous bone.
Sinus elevation bone grafting is a commonly performed procedure to increase maxillary bone height and width from the alveolar crest to the sinus floor for the support of one or more implants. Because of its osteogenic properties, autogenous bone remains the gold standard for this procedure and is the grafting material of choice for many surgeons.1,2 However, patients are often unwilling to accept this treatment method because of the added morbidity and potential complications associated with a second surgical procedure.
Bone allografts are obtained from human donors through tissue banks, accredited by the American Association of Tissue Banks, which screen, process, and store them under complete sterility.3,4 Allografts offer many advantages over autogenous bone grafts, including ready availability, avoidance of the need for a patient donor site, reduced time under anesthesia and in surgery, decreased blood loss, and fewer complications. Fresh allografts can be highly antigenic and generally are no longer used, but freezing or freeze-drying (lyophilizing) the bone significantly reduces the antigenicity.5
The adjunctive use of liquid PRP to promote healing and increase bone volume has become a standard part of many dental surgeons’ bone-grafting protocols, regardless of the grafting material used. PRP contains growth factors that are believed to facilitate osteogenesis as well as cell adhesion molecules that enhance osteoconduction.6 A more recent application of PRP has been developed to exploit these benefits in a configuration that also takes advantage of the scaffolding properties of PRP’s fibrin component, which serves as a kind of intercellular highway that platelets creep along to form bone.
This newer configuration, known variously as “Garg sticky bone™,” “sticky bone,” or “gummy bone,” is made by collecting the patient’s whole blood in a glass test tube and spinning it for an abbreviated cycle (about 3-4 minutes) to allow the components to separate but not to fully clot. The result is a middle layer of concentrated platelets, leukocytes, and fibrin that is then used to hydrate particulated bone, in this case freeze-dried bone allograft (FDBA). After about 15 minutes, clotting will be complete, and the result is “sticky bone.”
Excellent handling is the hallmark of Garg sticky bone™. Because it has the consistency of gummy bear candy, it can be easily molded into a surgical site and adapted to the shape of the bony defect. Furthermore, it maintains its 3D shape even after closure. The potency of sticky bone is excellent, providing approximately 5 times the baseline concentration of growth factors contained in whole blood.



Garg sticky bone™ can be used effectively in place of liquid PRP in sinus grafting, as shown in Figures 1 to 5. In this procedure, the lateral sinus wall is exposed via a broad-based, full-thickness mucoperiosteal flap, extending from the maxillary tuberosity to a releasing incision in the canine fossa region. The flap should extend superiorly to just below the infraorbital foramen to provide access to the lateral wall of the sinus. A large oval finishing bur or diamond bur is used to create an oval hole in the lateral cortical bone for access to the sinus membrane. To preserve its integrity, the sinus membrane is directly reflected in a series of stages, beginning at the sinus floor — superiorly, anteriorly, and posteriorly around the edges of the oval entry — until the sinus membrane is completely elevated posteriorly to the tuberosity. PRP sticky bone is introduced into the sinus to augment the alveolar ridge height. Note its excellent handling qualities. A PRP membrane can be used to close the oval window of the lateral sinus wall once the graft is in place.6
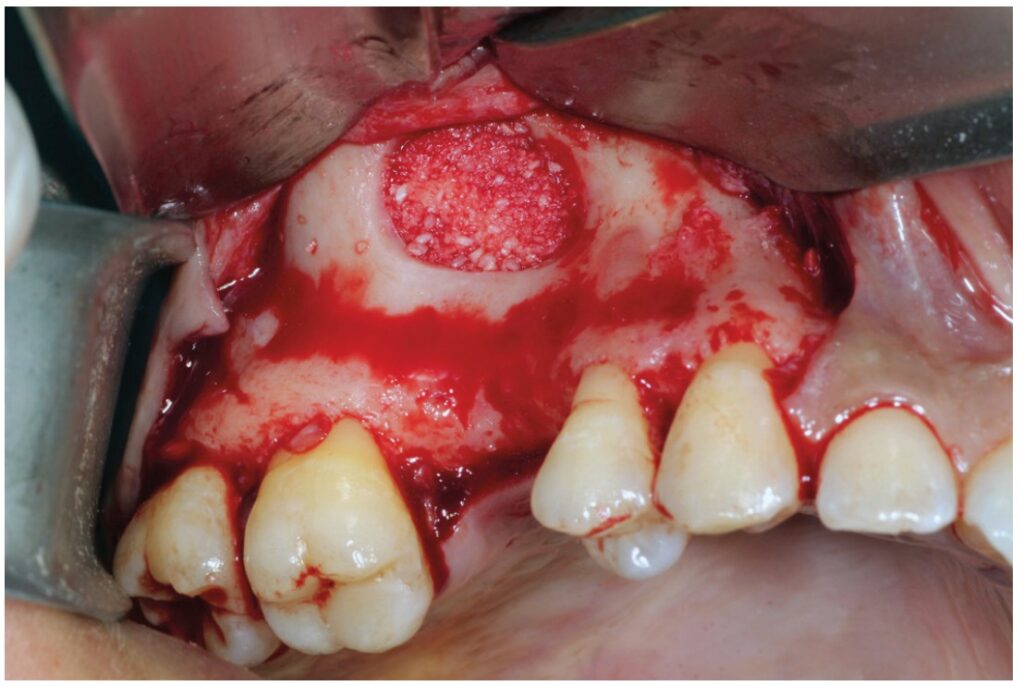

PRP’s growth factors enable the healing action of the endosteal osteoblasts and marrow stem cells that migrate from the bony sinus walls, while the allogeneic bone particles are bound by fibrin, fibronectin, and vitronectin, facilitating cell migration and bone regeneration. Using sticky bone in place of a standard bone graft makes this procedure easier and more predictable with accelerated healing.
Dr. Garg has discussed novel materials besides Garg sticky bone. Read “An innovative treatment option for rehabilitation of the atrophic anterior maxilla” for another interesting patient case. https://implantpracticeus.com/an-innovative-treatment-option-for-rehabilitation-of-the-atrophic-anterior-maxilla/
- Marx RE, Garg AK. Bone structure, metabolism, and physiology: its impact on dentalimplantology. Implant Dent. 1998;7(4):267-276.
- Marx RE, Armentano L, Olavarria A, Samaniego J. rhBMP-2/ACS grafts versus autogenous cancellous marrow grafts in large vertical defects of the maxilla: An unsponsored randomized open-label clinical trial. Int J Oral Maxillofac Implants. 2013;28(5):e243-e251.
- Malinin T, Temple HT. Comparison of frozen and freeze-dried particulate bone Cryobiology. 2007;55(2):167-170.
- Malinin TI, Carpenter EM, Temple HT. Particulate bone allograft incorporation in regeneration of osseous defects; importance of particle sizes. Open Orthop J. 2007;1:19-24.
- Sheikh Z, Hamdan N, Ikeda Y, et al. Natural graft tissues and synthetic biomaterials for periodontal and alveolar bone reconstructive applications: a review. Biomater Res. 2017;21:9.
- Garg AK. Autologous Blood Concentrates. 2nd ed. Quintessence Publishing; 2021.
Stay Relevant With Implant Practice US
Join our email list for CE courses and webinars, articles and mores



