Dr. Justin Moody offers tips on oral surgery in preparation for implants
People often ask me how much harder implant surgery is than oral surgery, and my answer is, It’s all really very similar. If you can remove a tooth, you can place a dental implant! The keys to oral surgery are fairly simple, and when you follow good surgical protocols, the procedures become efficient and predictable.
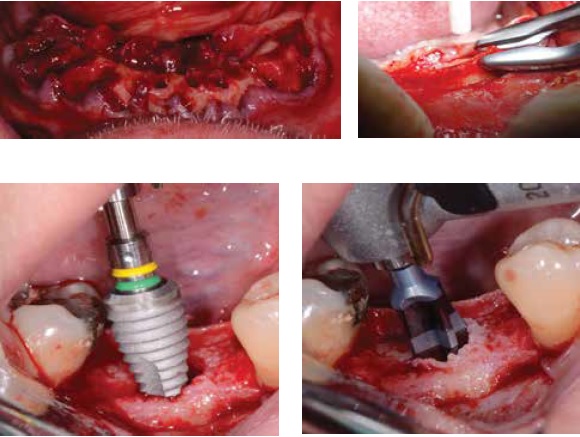
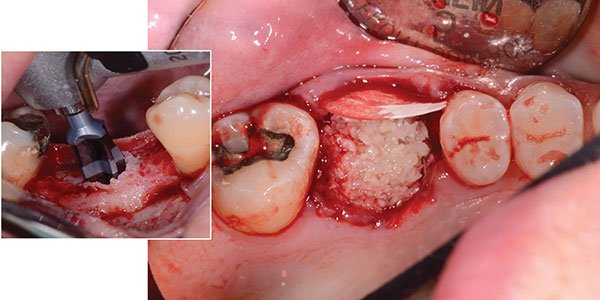
Access and visualization have always been key to good oral surgery; you can’t do quality work in the dark. Being able to visually see the site, whether it’s taking a tooth out, grafting a site, or placing an implant, is of the utmost importance. If you can remove teeth, you can place dental implants — it’s that simple. There is always an unknown with the extraction of teeth, curved roots, ankylosed teeth, or endodontically treated brittle teeth, for example. Dental implants do not have those issues. As a matter of fact, the whole process is much kinder to the patient both during and after the procedure.

Flap design and soft tissue maintenance is becoming the most important part of my procedures as the final cosmetic and long-term esthetic outcomes are directly dependent upon bone maintenance and tissue management. Creating flaps that have releasing incisions away from the surgical site, broad bases for good blood flow, and clean incisions significantly reduce the risk of complications. With the increased use of cone beam CT in dentistry, we can start to move away from large flaps and look for anatomical structures such as the mental foramen. The idea of working smarter, not harder, has taken on a whole new meaning.
Thankfully, today’s oral surgery is far less invasive, safer for the patient, and easier on the dentist. When implemented into the general dentistry practice, I find that the patient satisfaction is greatly increased from the decreased number of visits, and it’s good for revenue too! So get out there, and refresh your surgical skills by finding a good CE course or program — you won’t regret it!
Stay Relevant With Implant Practice US
Join our email list for CE courses and webinars, articles and mores

 Justin Moody, DDS, DICOI, DABOI, is a Diplomate of the American Board of Oral Implantology and of the International Congress of Oral Implantologists, Fellow and Associate Fellow of the American Academy of Implant Dentistry, and Adjunct Professor at the University of Nebraska Medical College. He is an international speaker and is in private practice at The Dental Implant Center in Rapid City, South Dakota. He can be reached at
Justin Moody, DDS, DICOI, DABOI, is a Diplomate of the American Board of Oral Implantology and of the International Congress of Oral Implantologists, Fellow and Associate Fellow of the American Academy of Implant Dentistry, and Adjunct Professor at the University of Nebraska Medical College. He is an international speaker and is in private practice at The Dental Implant Center in Rapid City, South Dakota. He can be reached at 

