Dr. Bart W. Silverman discusses how technology can result in more predictable treatment outcomes
Digital technology continues to revolutionize implant dentistry, benefiting every phase of the workflow. Integrating 3D digital technologies for comprehensive dentistry has advantages for both the treating dentist as well as our patients. The availability of cone beam computed tomography (CBCT) in the dental practice has made visualization of a patient’s anatomy prior to implant placement an invaluable tool when it comes to implant dentistry.
[userloggedin]
Guided surgical implant placement has allowed precise placement of implant restorations1 — we now start with a final predicted prosthetic result and work backwards, planning our cases with the end result in mind. With the use of a computer-manufactured resin guides, we now place our implants where they should be placed in order to restore our patients’ dentitions to a more predictable occlusion.
Intraoral digital scanning allows the treating dentist to digitally capture a patient’s occlusion and transfer that to a prosthetic center, where a temporary or final restoration can be computer milled. These computer-aided design/computer-aided manufactured, or CAD/CAM, restorations are then delivered to the patient with more exactness than before, thereby cutting down chair time and increasing profit margins. By combining these technologies, we have more predictable restorative outcomes that are clinically efficient for the doctors and take less time to final restoration for our patients.
Case overview
A 30-year-old male presented to the office following an altercation a few days prior when he reportedly was hit in the face with a barstool (Figure 1). The patient had a medical history, which was significant for stomach ulcers, and he was on dexilant medication with no known drug allergies. His oral and maxillofacial examination was significant for a horizontally fractured maxillary left lateral incisor. Our treatment plan included several options:
- endodontic therapy with possible extrusion, crown lengthening, post and core and crown;
- extraction, bone graft, delayed implant placement with possible soft tissue graft; or
- extraction, bone graft with immediate implant placement and load, with a temporary crown.
 One concern was provisionalization. If we chose to extract the tooth and place a bone graft with an immediate implant, we could place an immediate restoration, if insertional torque values warranted. If torque values were not sufficient for an immediate crown, then we could consider a Valplast®, an Essix appliance, or a bonded temporary bridge. If we chose to extract the maxillary left lateral tooth and bone graft for a delayed implant, a bonded or removable temporary prosthesis could serve as a provisional restoration. And finally, if we elected to do a fixed bridge without an implant, a temporary fixed bridge could be fabricated on the day of the extraction. We needed to consider the patient’s age, nature of injury, possible compliance with temporary restorations, and the preservation of hard and soft tissue architecture when deciding on our ultimate treatment plan.
One concern was provisionalization. If we chose to extract the tooth and place a bone graft with an immediate implant, we could place an immediate restoration, if insertional torque values warranted. If torque values were not sufficient for an immediate crown, then we could consider a Valplast®, an Essix appliance, or a bonded temporary bridge. If we chose to extract the maxillary left lateral tooth and bone graft for a delayed implant, a bonded or removable temporary prosthesis could serve as a provisional restoration. And finally, if we elected to do a fixed bridge without an implant, a temporary fixed bridge could be fabricated on the day of the extraction. We needed to consider the patient’s age, nature of injury, possible compliance with temporary restorations, and the preservation of hard and soft tissue architecture when deciding on our ultimate treatment plan.
There have been documented studies demonstrating that — when placing immediate implants into extraction sites — alveolar width and height can be preserved while reducing tissue loss and the need for subsequent soft tissue surgeries.2 After consultation with the patient and restorative dentist, we decided on immediate implant placement and temporary provisionalization, as this would allow for the best long-term prosthetic result.1 A guided surgical flapless approach would allow the implant to be placed where it ideally needed to be placed in order to create optimum prosthetics.2,3,4,5 Since we preoperatively knew where the implant would be placed, we fabricated a temporary abutment and temporary crown. They could be inserted at the time of implant placement and help maintain soft tissue contour and preserve the bony anatomy.1 A fixed temporary placed at the time of immediate implant placement would obviate the need for a removable prosthesis as well as reduce the overall time for case completion.
Treatment plan
 A preoperative cone beam scan with the CS 9300 system (Carestream Dental) was performed (Figure 2) as well as an intraoral digital impression using the CS 3500 intraoral scanner (Figures 3 and 4). Both files were sent to ROE Dental Labs in Garfield Heights, Ohio, where 3Shape’s Implant Studio™ software was used to plan a surgical guide, and their Dental Design system was used to fabricate the temporary abutment and crown. The temporary abutment was milled in PEEK acrylic material, and the temporary crown was milled out of A2 Shaded PMMA (Figures 5-10).
A preoperative cone beam scan with the CS 9300 system (Carestream Dental) was performed (Figure 2) as well as an intraoral digital impression using the CS 3500 intraoral scanner (Figures 3 and 4). Both files were sent to ROE Dental Labs in Garfield Heights, Ohio, where 3Shape’s Implant Studio™ software was used to plan a surgical guide, and their Dental Design system was used to fabricate the temporary abutment and crown. The temporary abutment was milled in PEEK acrylic material, and the temporary crown was milled out of A2 Shaded PMMA (Figures 5-10).
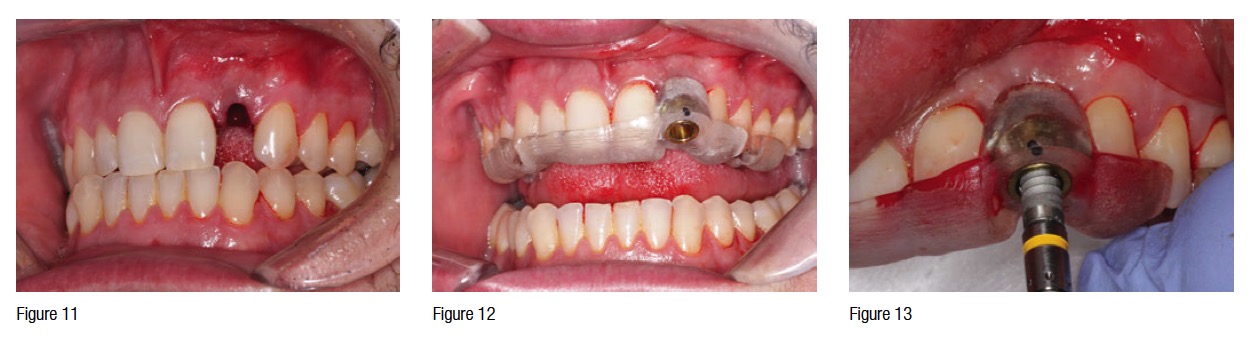
The patient was taken to the surgical operatory where blood pressure and pulse oximeter were placed, and an intravenous line was started. Anesthesia was maintained using a balanced technique. Local anesthesia was infiltrated to place with articaine 4% with epinephrine 1:100,000. The fractured maxillary left lateral incisor was atraumatically removed using appropriate elevators and forceps without raising a flap (Figure 11), and the surgical guide was placed and confirmed to be seated well in proper position (Figure 12). Using the BioHorizons® guided surgical kit and protocol, a 3.8 mm x 15 mm tapered internal implant was placed (Figures 13-14). Initial stability was confirmed and mineralized cortical bone placed in the buccal gap. An Osstell reading of 68 was obtained, and according to our loading protocol, the temporary custom-milled PEEK abutment was placed. The temporary crown was adjusted and cemented with a light rim of temporary cement (Figures 15-17).
Discussion
Planning the case with the end result in mind and working backwards and following the steps necessary to achieve this help provide an optimum result for our patients. Guided surgical placement of the implant allows for optimum positioning. Additionally, digital technology allows for the pre-op planning of a custom temporary abutment and crown, which can be placed at the surgical procedure. This immediate provisionalization allows for preservation of osseous and gingival tissues, as well as the guided tissue growth during the healing phase. Placing the implant immediately with same-day restoration decreases the number of surgical procedures and recovery time for our patients, while same-day temporization promotes ideal esthetics.
[/userloggedin]
[userloggedout][/userloggedout]
- Lazzara RJ. Immediate implant placement into extraction sites: surgical and restorative advantages. Int J Periodontics Restorative Dent. 1989;9(5);333-343.
- Rosenfeld AL, Mandelaris GA, Tardieu PB. Prosthetically directed implant placement using computer software to ensure precise placement and predictable prosthetic outcomes. Part 3: stereolithographic drilling guides that do not require bone exposure and the immediate delivery of teeth. Int J Periodontics Restorative Dent. 2006;26(5):493-499.
- van Steenberghe D, Glauser R, Blombäck U, Andersson M, Schutyser F, Pettersson A, Wendelhag I. A computed tomographic scan-derived customized surgical template and fixed prostheses for flapless surgery and immediate loading of implants in fully edentulous maxillae: a prospective multicenter study. Clin Implant Dent Relat Res. 2005;7(suppl 1):S111-S120.
- Abboud M, Wahl G, Guirado JL, Orentlicher G. Application and success of two stereolithographic surgical guide systems for implant placement with immediate loading. Int J Oral Maxillofac Implants. 2012;27(3):634-643.
- Sarment DP, Sukovic P, Clinthorne N. Accuracy of implant placement with a stereolithographic surgical guide. Int J Oral Maxillofac Implants. 2003;18(4):571-577.
Stay Relevant With Implant Practice US
Join our email list for CE courses and webinars, articles and mores